|
8/12/2023 0 Comments Pinpoint rash with itching 
7 However, in the first months after the diagnosis, several drugs can be used. Treatment of dermatitis herpetiformis is based on a gluten-free diet for life, which leads to healing of the rash and enteropathy. 6 Serological tests, such as anti-transglutaminase and anti‑endomysial antibodies, have high specificity and sensitivity for dermatitis herpetiformis, and are a useful adjunct for diagnosis. 1,5 Thus, to make a diagnosis, biopsies in two different locations – one from lesional skin for routine histopathology and another from perilesional skin for DIF – should be taken: DIF will show deposits of IgA with epidermal transglutaminase complexes in the papillary dermis. Routine histopathology of a dermatitis herpetiformis skin lesion showing an inflammatory infiltrate mainly composed of neutrophils is not diagnostic, as other bullous diseases may show similar findings. The diagnosis of dermatitis herpetiformis relies on skin biopsy results. 5 Some patients also describe a personal or family history of other autoimmune disorders such as Hashimoto’s thyroiditis, pernicious anaemia, type 1 diabetes mellitus and alopecia areata. 6 There is an association with human leukocyte antigens (HLA) DQ2 and DQ8. 
5 A diet containing gluten causes the development of immunoglobulin A (IgA) antibodies against gluten-tissue transglutaminase, which is found in the gut, leading to a cross-reaction between these antibodies and epidermal transglutaminase. 3 The pathophysiology of dermatitis herpetiformis involves gluten as an environmental trigger, genetic factors and dysregulation of the immune system. 4 Among patients with coeliac disease, 15–25% will develop dermatitis herpetiformis. 2 The majority of patients with dermatitis herpetiformis have evidence of coeliac disease, but less than 10% have symptoms or signs of malabsorption. The most likely diagnosis is dermatitis herpetiformis, which is the result of an immunological response of the gut mucosa to persistent stimulation by dietary gluten. The main diagnoses to be taken into account in this patient are listed in Table 1. What is the appropriate management of this condition and prognosis? Answer 1 How is this condition diagnosed? Question 4 What is the most likely diagnosis and aetiology of this condition? Question 3 What differential diagnoses should be considered in this case? Question 2 Four punch biopsies of lesional and perilesional skin from the arms and buttocks were taken for routine histopathology and direct immunofluorescence (DIF).įigure 1. 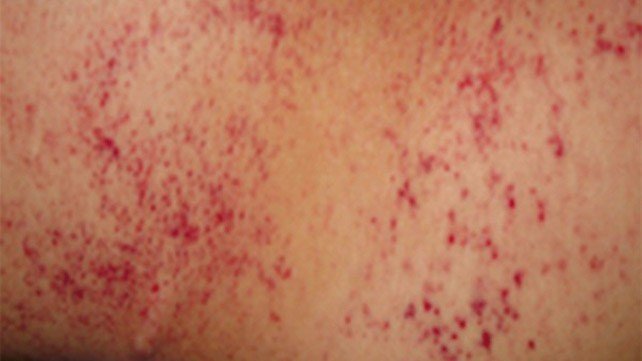
The patient was otherwise healthy and denied any history of fever, photosensitivity or symptoms in other family members. The patient reported a loss of approximately 5 kg in weight, and several episodes of diarrhoea and abdominal discomfort in the previous year. Some of the lesions were excoriated with bloodstained crusting. The rash was characterised by clusters of translucent, tense vesicles located symmetrically on the extensor surfaces of the arms and legs (Figure 1A, B), and by erythematous papules and small plaques on the buttocks (Figure 1C). A man, 30 years of age, presented with an intensely pruritic eruption that had been evolving for approximately two months. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
